 Ngày đăng: 09/04/2026Tác giả: Nguyen Thi Ngoc, Le Doan Tri, Tran Duc Huy, Nguyen Ha
Ngày đăng: 09/04/2026Tác giả: Nguyen Thi Ngoc, Le Doan Tri, Tran Duc Huy, Nguyen HaHepatobiliary diseases, ranging from benign lesions to liver cancer, are on the rise in Vietnam, particularly against the background of viral hepatitis and chronic liver diseases. In this context, early detection and accurate characterization of lesions are decisive factors for effective treatment. Magnetic resonance imaging (MRI) of the liver and biliary system using hepatocyte-specific contrast agents at Bach Mai Hospital is considered a significant advancement, contributing to improved diagnostic accuracy.
A “Key” to Clearly Identifying Liver Lesions
Magnetic resonance imaging (MRI) is a modern diagnostic modality that uses magnetic fields and radio waves to generate detailed images of internal organs without the use of ionizing radiation.
In hepatobiliary evaluation, the use of hepatocyte-specific contrast agents provides superior value. Unlike conventional contrast agents, these agents are selectively taken up by hepatocytes and excreted through both the biliary system and kidneys.
As a result, the technique not only provides structural imaging but also reflects the functional status of liver cells and the biliary system—an especially important factor in characterizing lesions.
MRI imaging of a patient’s hepatobiliary system using a hepatocyte-specific contrast agent
Improved Early Detection of Cancer and Small Lesions
According to experts from the Department of Diagnostic and Interventional Radiology, MRI with hepatocyte-specific contrast agents enables comprehensive assessment across both vascular dynamic phases and the hepatobiliary phase after contrast administration, allowing for a thorough evaluation of lesions.
A key advantage of this method is its ability to detect very small liver lesions, including those that may be missed by CT scans or conventional MRI. Notably, it facilitates clear differentiation between benign lesions (such as focal nodular hyperplasia and hepatic adenoma) and malignant tumors such as hepatocellular carcinoma (HCC).
Additionally, the technique is valuable in detecting liver metastases, evaluating the biliary system, and guiding individualized treatment strategies.
Several studies have shown that for lesions ≤2 cm, MRI using hepatocyte-specific contrast agents can achieve a sensitivity of approximately 87%, higher than that of CT (around 73%). Clinical research has also reported that this technique can detect additional lesions in about 16% of patients, potentially altering disease staging and enabling curative treatment options such as tumor ablation, liver resection, or transplantation.
Standardized Procedures Ensuring Safety
At Bach Mai Hospital, MRI procedures using hepatocyte-specific contrast agents are conducted under strict standardized protocols. Patients undergo medical history assessment, indication evaluation, removal of metallic objects, and preparation for intravenous access.
The imaging process includes baseline sequences prior to contrast injection, followed by administration of the contrast agent and acquisition of images at multiple phases, particularly the hepatobiliary phase approximately 15–20 minutes post-injection. All imaging data are processed and interpreted by specialized radiologists.
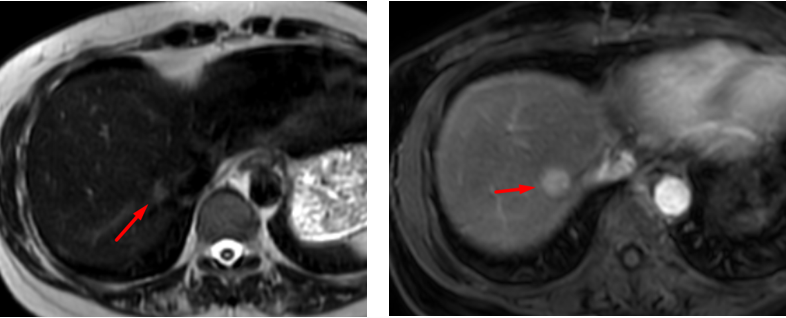
Indeterminate liver lesion on conventional MRI
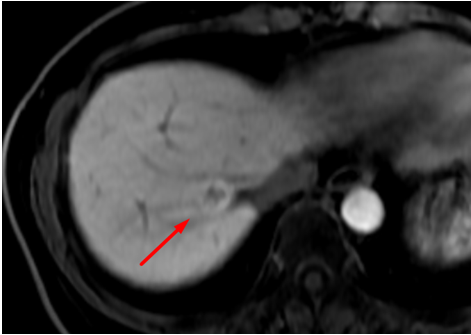
Liver lesion demonstrating retention of hepatocyte-specific contrast agent in the hepatobiliary phase, suggestive of focal nodular hyperplasia (FNH).
High Safety Profile and Impact on Treatment Strategy
One of the key advantages of this technique is that it does not use ionizing radiation, thereby eliminating radiation exposure for patients. Hepatocyte-specific contrast agents have a low rate of adverse effects, which are generally mild and transient. However, in patients with severe liver or kidney impairment, their use should be carefully considered under specialist guidance.
Clinical practice has demonstrated that MRI with hepatocyte-specific contrast agents not only improves diagnostic accuracy but also plays an important role in selecting treatment modalities, monitoring disease progression, and evaluating post-intervention outcomes.
In particular, for assessing liver metastases from colorectal cancer, this technique enables surgeons and oncologists to develop more precise treatment plans. Some studies indicate that it can lead to changes in treatment modality in approximately 18% of cases and adjustments in the extent of local interventions in about 20% of cases.
With modern equipment and a highly experienced team of physicians, Bach Mai Hospital has effectively implemented this technique in clinical practice. This represents a significant advancement in diagnostic imaging, contributing to improved treatment quality and better prognostic outcomes for patients with hepatobiliary diseases.