 Ngày đăng: 25/03/2026Tác giả: Nguyen Ha - The Anh
Ngày đăng: 25/03/2026Tác giả: Nguyen Ha - The AnhWhat began as a fleeting episode of mild chest discomfort led a 44-year-old man to walk into Bach Mai Hospital “just for reassurance.” Within minutes, however, he suffered a sudden cardiac arrest at the A9 Emergency Center. Thanks to timely resuscitation, he survived and made a near-complete recovery. The case serves as a stark warning about fulminant myocardial infarction in younger individuals—and, above all, highlights the professionalism and dedication of Bach Mai physicians who acted swiftly to save a life.
A “Mild” Pain, a Sudden Collapse, and the Start of a Life-or-Death Race
Mr. Nguyen Van S. (44, from Hai Phong), the breadwinner of a family with four young children-the youngest not yet two years old-works with his wife at a restaurant in Hanoi to support the family. With no prior personal or family history of cardiovascular disease, he never imagined he could be at risk. “I thought it was just fatigue from work or maybe smoking affecting my lungs,” he shared.

Assoc. Prof. Dr. Dao Xuan Co and the medical team congratulate the patient on the day of discharge
On the afternoon of March 17, he experienced mild chest tightness and considered seeking medical attention but delayed due to work. By around 7:00 PM, the pain intensified, coming in intermittent sharp episodes. He then went alone to the A9 Emergency Center at Bach Mai Hospital for evaluation, assuming it was a routine check-up.
Upon arrival, he underwent initial assessment and was ordered diagnostic tests. However, immediately after a blood sample was drawn, he suddenly lost consciousness and collapsed, leaving bystanders shocked.
Dr. Tran Hoai Linh, the attending emergency physician, recalled: “Everything happened very quickly. As soon as the patient lost consciousness and collapsed, our staff supported him and called for assistance. Within about 10 seconds, he was placed on a stretcher, transferred to the resuscitation area, and chest compressions were initiated immediately.”
What followed was a full-scale, coordinated resuscitation effort: chest compressions, defibrillation, medications, endotracheal intubation, urgent laboratory testing, and cardiology consultation-all performed simultaneously with precision and teamwork. After three defibrillation shocks and 15 intense minutes of resuscitation, his pulse returned and spontaneous circulation was restored.
“Normal” Yet Not Normal: A Warning Sign of a Dangerous Condition
What puzzled the medical team was that the patient’s vital signs were initially stable, and early test results showed no clear evidence of coronary artery disease or myocardial infarction. Under such circumstances, patients are often discharged with outpatient follow-up.
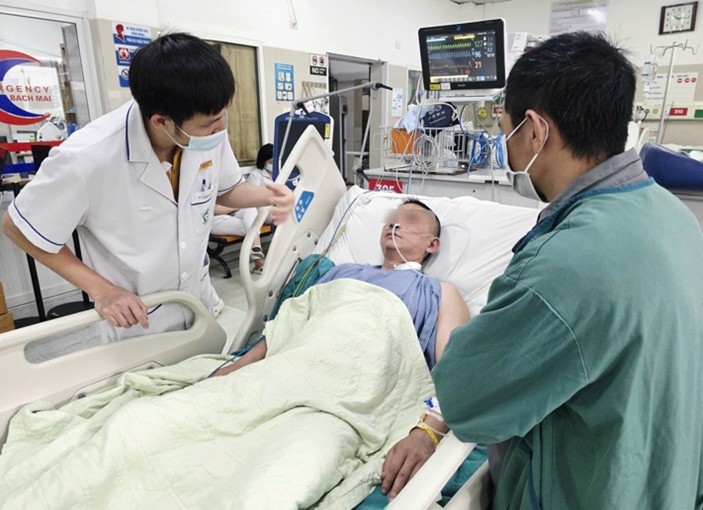
The patient was closely monitored by doctors, with every vital parameter carefully tracked
However, given their clinical experience-especially in a relatively young patient without obvious risk factors and with non-specific ECG and cardiac enzyme findings-the team decided to pursue further investigation.
Coronary angiography was performed to identify the root cause. The findings revealed a myocardial bridge of the left anterior descending artery (LAD) with up to 99% stenosis in the segment distal to the bridge. This was the underlying cause of malignant ventricular arrhythmia leading to sudden cardiac arrest.
Assoc. Prof. Nguyen Anh Tuan, Director of the A9 Emergency Center, explained: “This was a case of evolving myocardial ischemia, presenting with malignant ventricular arrhythmia before cardiac biomarkers became elevated. The first manifestation of severe disease was ventricular fibrillation leading to cardiac arrest. Had the patient not been in the hospital, or had the emergency team not responded promptly, the likelihood of death would have been extremely high.”
Critical Moments and an Unexpectedly Positive Outcome
The patient underwent immediate coronary stenting, followed by intensive care management, including targeted temperature management for 48 hours, sedation, mechanical ventilation, hemodynamic support, and risk factor control.
After completion of therapeutic hypothermia, he regained consciousness, was successfully extubated, and made a full recovery without neurological deficits.
“When we saw him again, he was fully conscious, with almost no neurological sequelae. That’s not something every case achieves,” the doctors shared emotionally.
On the day of discharge, smiles returned to the faces of his wife, father, relatives, and friends. “When I heard he had collapsed, I felt weak and panicked. He is the pillar of our family—without him, I don’t know how we would cope. We are so fortunate he came to the hospital in time. Just a few minutes later, or if he hadn’t gone at all, things could have been very different,” his wife said tearfully.
Spreading Resuscitation Skills – Creating More Chances for Survival
At the discharge, witnessing the family’s reunion, Assoc. Prof. Dao Xuan Co, Director of Bach Mai Hospital, emphasized that this outcome reflects high professional expertise, seamless teamwork, effective multidisciplinary collaboration, and, above all, the medical ethics and dedication of healthcare workers.

Assoc. Prof. Dr. Dao Xuan Co delivers remarks at the event, commending the medical team and congratulating the patient and their family
He stressed: “If the community is equipped with basic cardiac arrest response skills, many more lives could be saved instead of waiting until hospital arrival. The A9 Emergency Center and Bach Mai Hospital should continue to promote and expand community training in basic life support-guiding people on how to perform chest compressions and provide initial first aid. In such situations, the ‘golden hour’ waits for no one. When people know how to act, we can create thousands more survival opportunities like that of Mr. S.”
As Mr. S. left the hospital, it was not a scene of sorrow, but one filled with laughter and renewed hope as his family continues their journey together.
|
Important Reminders:
|