 Ngày đăng: 19/03/2026Tác giả: Nguyen Ha
Ngày đăng: 19/03/2026Tác giả: Nguyen Ha
Doctors at Bach Mai Hospital have successfully saved the life of a patient with complex maxillofacial trauma, including a ruptured left eyeball caused by a metallic foreign object to the face. The outcome highlights not only the Hospital’s clinical expertise and strong sense of professional responsibility, but also the urgent, well-coordinated collaboration across multiple specialties—a core strength of Bach Mai Hospital in the management of severe and complex cases.
At Bach Mai Hospital, the operating rooms of the Department of Anesthesiology and Critical Care remain active throughout the night. Yet on the evening of March 13, the pressure was particularly intense as doctors from Maxillofacial Surgery, Otorhinolaryngology, Ophthalmology, Plastic and Reconstructive Surgery, Neurosurgery, and Anesthesiology urgently coordinated to save a patient with severe facial trauma caused by a metallic object penetrating the left orbital cavity.
The case was exceptionally complex, with critical risks present at every step of the procedure. For the 44-year-old man, death remained a real possibility at any moment during surgery.
Following more than three hours of determined, high-stakes intervention, the operation was successful, and the patient’s life was preserved.
A life-altering accident from a snapped chain
The patient, a 44-year-old male container truck driver with no previous medical history, recalled that at around 11:30 a.m. on March 13, he and a colleague were traveling through Ky Son, Hoa Binh Province, when heavy rain caused his colleague’s vehicle to become stuck in the mud.
In an attempt to pull the vehicle free, he used a metal chain to connect the two trucks. During the process, the chain suddenly snapped, and a fragment of metal was forcefully propelled into his face, even though he was standing about 20 steps away. After receiving initial first aid at a local medical facility, he was urgently transferred to Bach Mai Hospital.
Upon arrival at Emergency Center A9, the patient remained conscious. However, his left eye was heavily bandaged and soaked with blood, while the metallic object was still lodged in the left side of his face and eye.
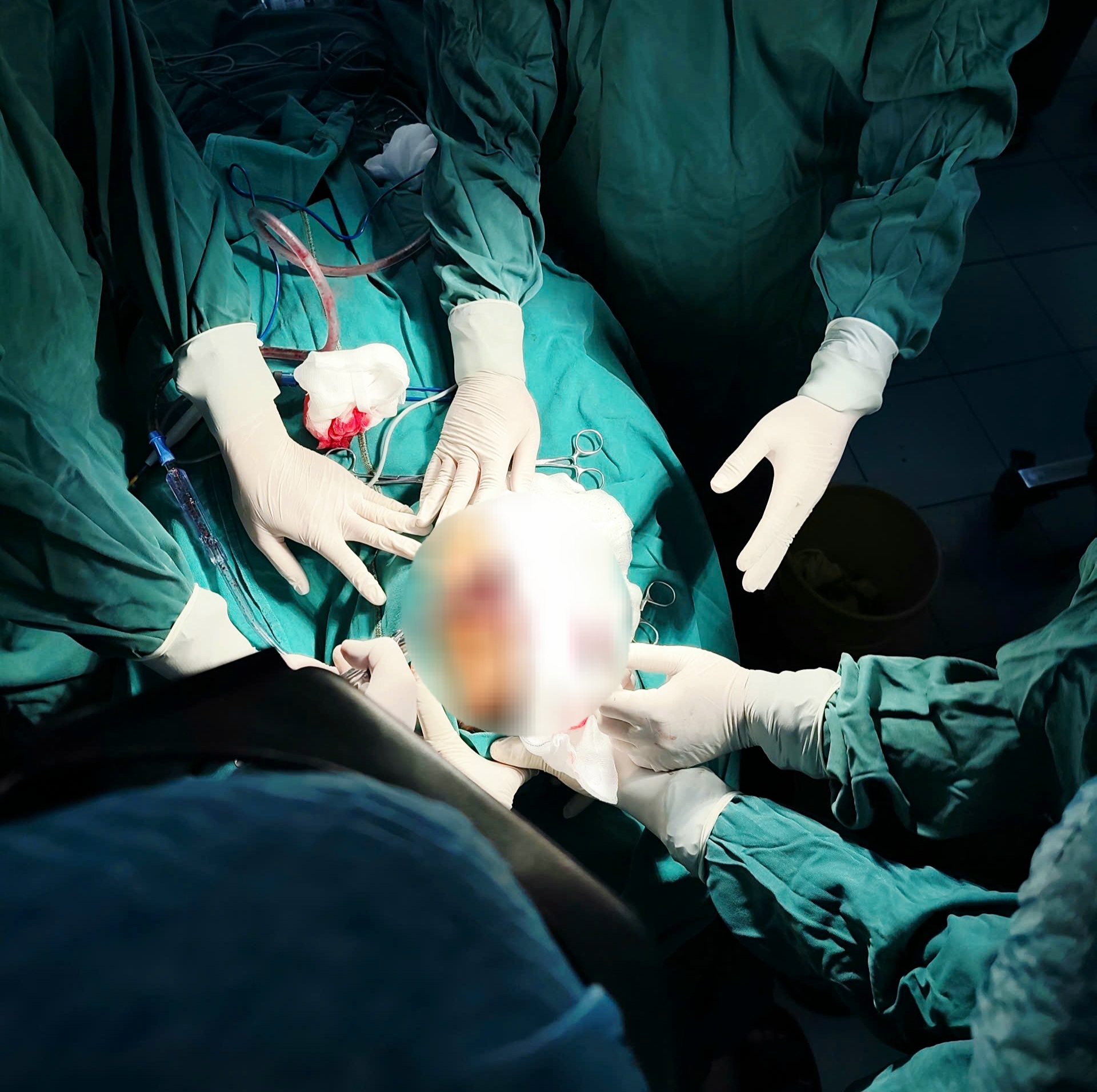
The process of removing the foreign object from the patient
CT scans showed extensive and severe trauma, including a fractured left zygomatic bone, complete destruction of the orbital wall, deformity of the left eyeball, multiple sinus fractures, bilateral nasal bone fractures, and widespread swelling, hematoma, and subcutaneous emphysema.
The patient was quickly diagnosed with complex maxillofacial trauma, rupture of the left globe, and a retained metallic foreign body—a life-threatening condition that could worsen at any time.
A High-Risk Decision: Emergency Surgery Through the Night
At 9:30 p.m. that same day, an urgent hospital-wide consultation was convened, bringing together specialists in anesthesiology, maxillofacial surgery, otorhinolaryngology, ophthalmology, neurosurgery, and plastic surgery.
Despite the extremely high risk of rapid deterioration and death, the multidisciplinary team reached a unanimous decision to proceed with emergency overnight surgery in an effort to remove the foreign body, control bleeding, manage the complex injuries, and save the patient’s life.
Even before the operation began, major challenges were already apparent. Because of airway obstruction caused by bleeding, the patient was unable to breathe through his nose and had to rely entirely on mouth breathing. Severe facial swelling further limited mouth opening. In addition, his stomach was full, significantly increasing the risk of aspiration and making airway management exceptionally difficult.
As one anesthesiologist recalled, “This was an extremely complex case with unpredictable risks, including difficult intubation, possible ventilation failure, the potential need for tracheostomy, uncontrolled bleeding, skull base collapse, cerebrospinal fluid leakage, and even death during anesthesia. However, in order to save the patient, we decided to perform awake intubation.”
Inside the operating room, every second was critical. The patient was carefully instructed and encouraged to cooperate throughout the procedure. However, during intubation, he repeatedly vomited both fresh blood and dark blood. The first attempt failed. The second attempt also failed. Only on the third attempt was the endotracheal tube successfully and safely inserted, securing the airway and making it possible for the surgical team to proceed.
A life-and-death battle in the operating room
From that moment on, a true life-and-death battle unfolded in the operating room. The surgical teams worked in close coordination, taking turns to remove the deeply embedded metallic foreign body, excise the ruptured left globe, clean the damaged cavities, and reconstruct the facial structures.
The greatest challenge lay in accessing the foreign object, which was lodged deep within the bony structures and paranasal sinuses. Every maneuver carried a substantial risk of severe bleeding. At several points during the operation, the patient’s heart rate dropped to just 20–25 beats per minute, while his blood pressure fell to critically low levels and responded poorly to medication. The procedure had to be temporarily paused so that the team could stabilize his vital signs before continuing.
As one ENT surgeon recalled, “At those moments, it felt as though the entire operating room was holding its breath.”
After more than three hours of intense and high-stakes effort—from 1:30 a.m. to 4:40 a.m. on March 14—the surgical team successfully removed all foreign bodies, including a metal fragment nearly 6 cm in length that had penetrated the orbital cavity.
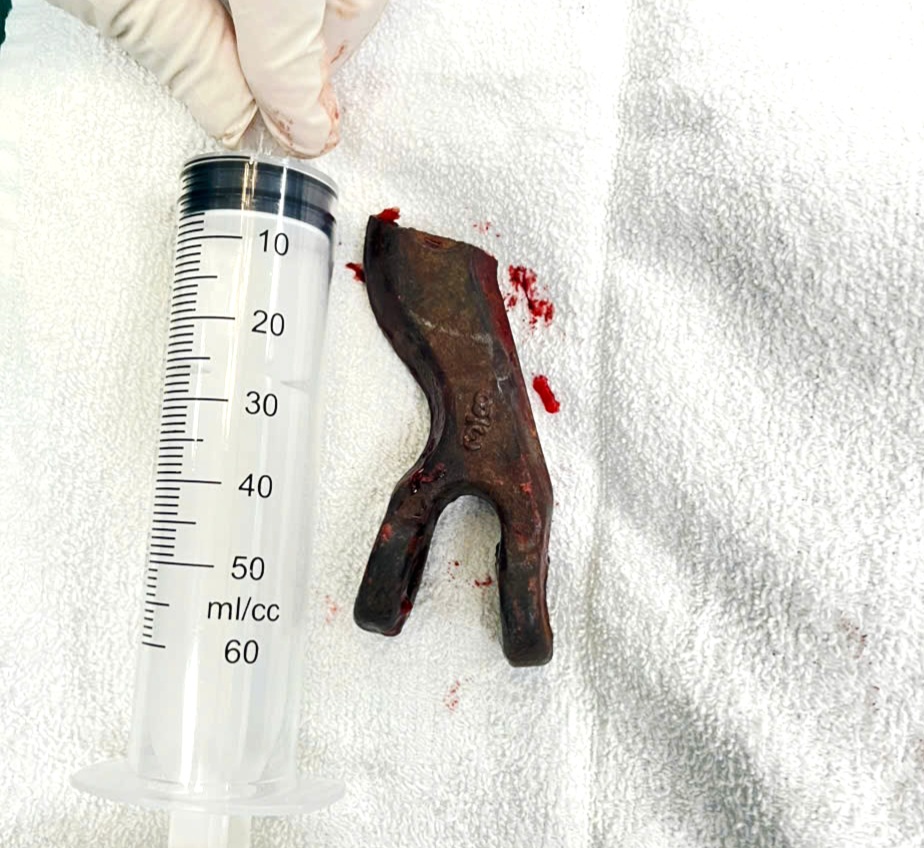
The foreign object removed from the patient’s left eye socket
The Strength of Multidisciplinary Coordination — A Defining Feature of Bach Mai Hospital
The success of the surgery was not the achievement of any one individual, but the result of close, highly coordinated collaboration among multiple specialties. Every decision required careful consensus, and every intervention depended on seamless teamwork. In a case where the boundary between life and death was exceptionally fragile, multidisciplinary coordination was not simply an advantage—it was a decisive factor in saving the patient’s life.
Outside the operating room, the patient’s wife was overcome with distress upon learning of the accident. Through tears, she shared, “He is the main breadwinner of our family, and we have two young children. I do not know what we would do if anything happened to him.”
The challenges did not end after surgery. When the patient regained consciousness and learned that he had lost one eye, he was devastated. As a long-haul driver, he suddenly faced the loss of his livelihood and deep uncertainty about the future. Overwhelmed by the shock, he fell into emotional crisis and initially refused further treatment.
In the days that followed, however, the dedication and compassion of the medical team became an important source of emotional support. Through patient explanation, reassurance, and constant encouragement, both the patient and his wife gradually came to accept the reality of the situation and began to regain hope.
Expressing her gratitude, the patient’s wife said, “We are deeply grateful to the doctors. They not only saved my husband’s life, but also helped him stand up again after this devastating shock.”

Doctors from the Department of Anesthesiology and Critical Care, Bach Mai Hospital, examine the patient after surgery
Where Medical Ethics and Professional Excellence Converge
The patient is currently receiving care in the Surgical Intensive Care Unit under the Department of Anesthesiology and Critical Care at Bach Mai Hospital. He has passed the most critical phase, his condition is stable, and he has regained mobility.
This case stands as a clear testament to Bach Mai Hospital’s capacity to manage complex medical emergencies—a place where advanced expertise, high-level technical capability, professional responsibility, and multidisciplinary coordination come together to save lives.
More than that, it is also a story of the people behind the operating table—those who remained awake through the night, working under immense life-and-death pressure to preserve a patient’s life. At a moment when every factor seemed to weigh against them, it was their coordination, resilience, and unwavering medical ethics that made the seemingly impossible possible.
And beyond the doors of the operating room, one family has been given hope once again.